Common blood tests may offer early detection of bone loss, with recent research indicating that alkaline phosphatase (ALP) levels could serve as a useful marker for identifying individuals who might benefit from earlier osteoporosis assessments. A study published in the journal Frontiers in Endocrinology explored the correlation between ALP levels and osteoporosis risk, revealing significant associations that warrant further investigation.
The study identified that elevated ALP levels are strongly linked to a higher probability of osteoporosis, especially in metabolically healthy, younger, and female participants. This finding suggests a potential threshold for recommending additional bone health evaluations, aiming to prevent fractures before they occur.
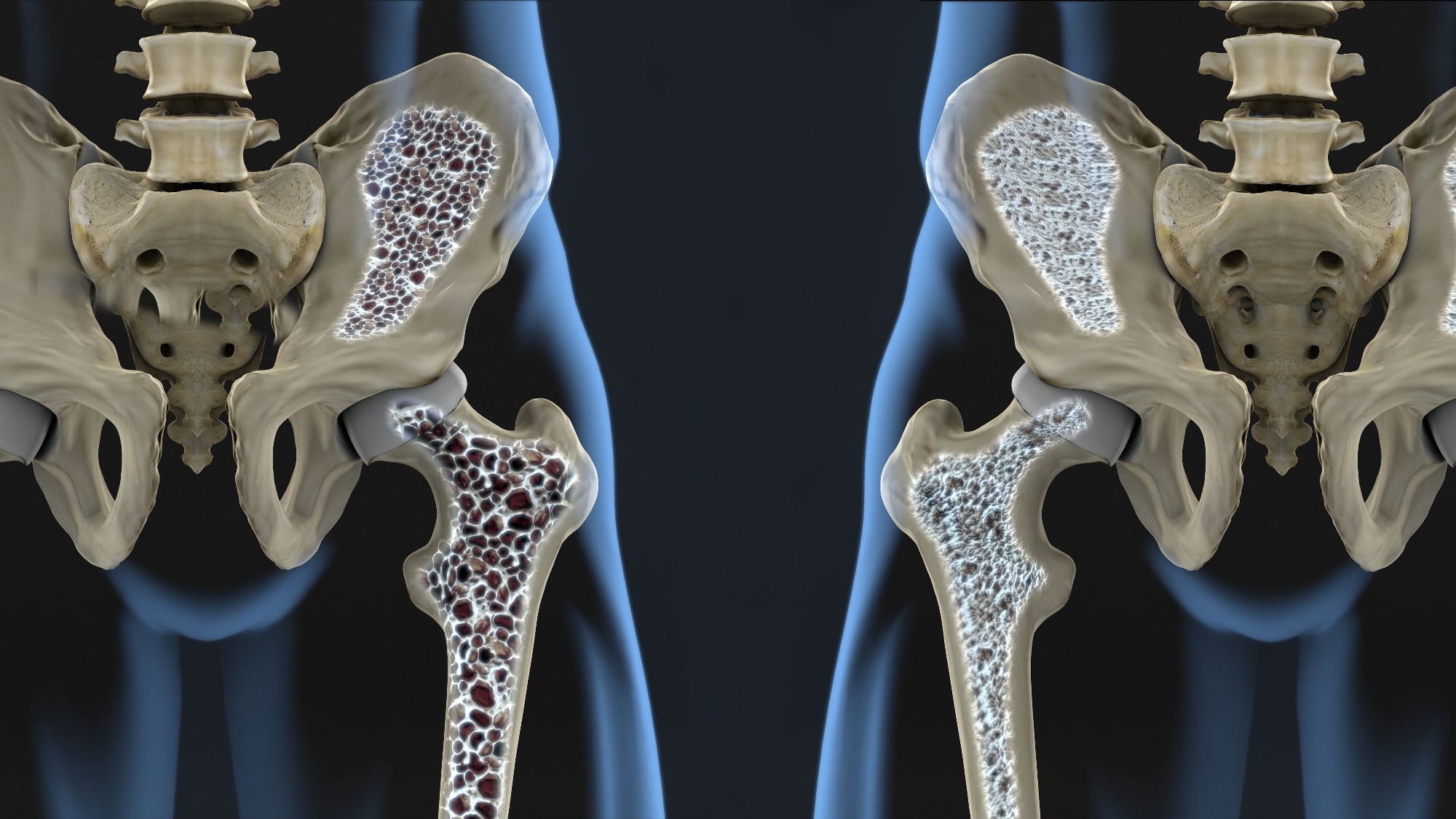
Osteoporosis, marked by decreased bone mass and structural degeneration, leads to a heightened fracture risk and adversely affects health and quality of life. With global life expectancies on the rise, the prevalence of osteoporosis is increasing, particularly in individuals over 75. The need for accessible biomarkers to detect bone loss early is critical.
ALP, primarily produced by bone-forming osteoblasts and hepatocytes, plays an essential role in bone mineralization by breaking down pyrophosphate. Approximately half of the ALP in the bloodstream originates from bones, and bone-specific ALP levels align closely with total ALP levels in both healthy and osteoporotic individuals.
Total ALP is inexpensive and widely available in routine health checks, yet previous studies have shown inconsistent results regarding its efficacy as a bone health marker. Variations in sample size, population diversity, and the influence of metabolic or liver conditions on ALP levels complicate interpretation.
The research was conducted using cross-sectional data from routine health examination records at a large teaching hospital in Chongqing, China, covering the period from 2019 to 2024. Participants were adults aged 20 or older who underwent both blood ALP testing and dual-energy X-ray absorptiometry (DXA) scans. The study adhered to World Health Organization (WHO) criteria for osteoporosis diagnosis, utilising DXA T-scores, with modifications for younger adults.
Statistical analyses comprised descriptive comparisons, t-tests, chi-square tests, and logistic regression models, adjusting for age, sex, body composition, metabolic markers, and liver function. The analysis confirmed a mostly linear relationship between ALP levels and osteoporosis risk, although the association weakened when ALP levels exceeded 100 IU/L. A receiver operating characteristic (ROC) analysis identified 72 IU/L as the optimal cut-off for predicting osteoporosis.
Subgroup analyses revealed stronger statistical associations in women, younger individuals, and those with normal liver enzymes and healthier metabolic profiles. In contrast, elevated liver enzymes or abnormal glucose or lipid profiles significantly weakened or nullified the association, indicating that metabolic and hepatic factors may distort the relationship between ALP levels and bone health.
The study concludes that higher serum total ALP is consistently associated with an increased likelihood of osteoporosis, even within normal reference ranges and after accounting for various confounders. The association is most pronounced in younger women and metabolically healthy individuals, likely due to ALP more accurately representing bone-derived ALP when liver and metabolic functions are normal.
While the study’s strengths include a large sample size and standardized clinical data, its cross-sectional design, single-centre population, and lack of data on physical activity, thyroid status, medication use, and diet limit the findings. Further longitudinal studies are necessary to confirm the causal and predictive value of ALP levels as a marker for osteoporosis risk.